Women and the Prostate Gland: What You Need to Know
Understanding the Female Prostate: Functions, Myths, and Medical Insights

Curious whether a “female prostate” exists and what it means for health? Many readers ask do women have prostate glands when they learn about the male prostate and cancer risks.
The male prostate is a walnut-shaped organ tied to producing prostatic fluid and to reproduction. Researchers compare those secretions to similar female structures called Skene’s glands, which some call the female prostate.
Prostate cancer is common in men, with about one in eight males diagnosed in their lifetime. Understanding rare cancers in the female anatomy helps spot early signs, like changes in PSA or unusual symptoms, and supports better care for all people.
Key Takeaways
- The phrase “female prostate” often refers to Skene’s glands.
- Male prostate makes fluid and is central to male reproduction.
- Prostate cancer mainly affects men but rare forms can appear in females.
- High PSA levels can signal prostate cancer in males.
- Knowing anatomy helps with early detection and informed care.
Understanding the Anatomy: Do Women Have Prostate Glands?
Short answer: Certain small structures near the female urethra are often compared to the male prostate, but they are not the same organ.
The term female prostate usually refers to Skene’s glands. These glands sit near the urethral opening and are part of the urogenital system. Their tissue shares embryologic origins with the male prostate, which helps explain the comparison.
Anatomically, the male prostate sits just below the bladder and surrounds the top of the urethra. That location differs from the area where Skene’s tissue is found in females. This difference matters for how certain urologic conditions present and are evaluated.
- Skene’s are a small but important part of urethral and pelvic health.
- Shared developmental tissue explains biochemical similarities.
- Common male diagnoses like prostatitis have distinct counterparts in female anatomy.
Understanding these parallels helps patients and clinicians monitor urinary and reproductive health across sexes. Clear anatomy guides better screening and care for both men and females.
The Role and Function of Skene Glands
Embryological roots explain why small paraurethral tissue resembles male structures.
Origins in Development
The Skene structures come from the urogenital sinus, the same embryonic tissue that forms the male prostate. This shared origin explains similar cell types and biochemical markers.
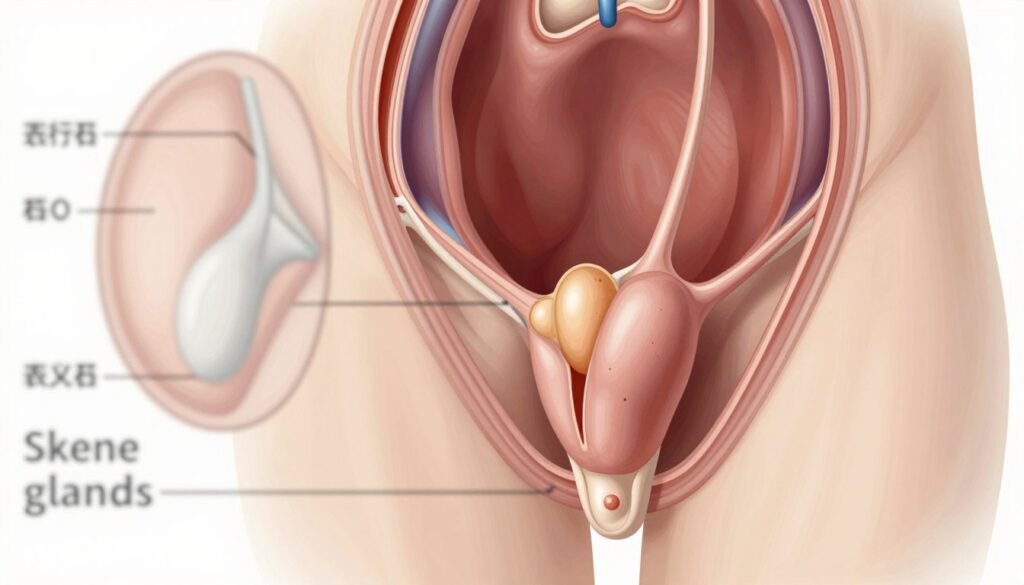
Secretory Functions
Skene glands produce fluid that supports local urogenital health. Lab studies show they release prostate-specific antigen and prostatic acid phosphatase, markers once thought exclusive to the male prostate.
- Located on the anterior vaginal wall near the lower urethra, these structures act as a secretory unit.
- They contribute to lubrication and may influence local microbial balance and comfort.
- Their PSA production is a biochemical link to the male prostate and a subject of ongoing research.
| Feature | Skene Structures | Male Prostate |
|---|---|---|
| Embryologic origin | Urogenital sinus | Urogenital sinus |
| Location | Anterior vaginal wall near urethra | Below bladder, surrounds urethra |
| Secretions | PSA, PAP, lubricating fluid | Prostatic fluid, PSA, PAP |
| Clinical relevance | Rare neoplasms; diagnostic interest | Common site of cancer and PSA screening |
Clinical Perspectives on Female Prostate Cancer
Though extremely rare, cancers arising from paraurethral tissue pose real clinical challenges.
Reports show how unusual presentations can delay diagnosis. Clinicians rely on a mix of imaging, lab markers, and tissue review to reach a clear answer.
Symptoms and Diagnostic Challenges
Common signs include pelvic pain, a palpable mass, or blood in the urine. Such symptoms often mimic benign urethral or reproductive conditions.
Diagnostic clues may include elevated prostate-specific antigen or abnormal imaging. A 2022 review in Frontiers in Oncology reported only about twenty documented cases in medical history.
- Pathology may show patterns rated with a Gleason score such as 4+4 on microscopic review.
- Treatment typically involves surgical removal, sometimes labeled as a prostatectomy, followed by radiation or systemic therapy.
- Because incidence is so low compared with men, misdiagnosis is common and careful follow-up matters for long-term health.
Exploring the Connection Between the G-Spot and Female Prostate
Ernst Gräfenberg first described the G-spot in 1950 as a sensitive area on the anterior vaginal wall.
Modern research links that region to nearby paraurethral tissue. Anatomical studies note the area near the bladder neck can be highly sensitive. This region is a functional part of sexual response for many people.
A 2022 review suggested sensations labeled as the G-spot may stem from stimulation of the skene glands. These structures sit beside the urethra and consist of secretory tissue that some call the female prostate.
About 40.9% of people report orgasm from both clitoral and vaginal stimulation, showing that multiple areas contribute to pleasure. While the male prostate is a distinct organ, paraurethral units act as an analogous part in pelvic anatomy.
- G-spot sensations often map to the anterior wall near the bladder neck.
- Stimulation likely involves sensitive urethral-adjacent tissue rather than a single organ.
- Clearer anatomy helps guide sexual health conversations and clinical care.
Conclusion
Recognizing uncommon cancers near the urethra can speed diagnosis and improve outcomes. Skene’s tissue acts as a functional equivalent to the prostate gland, though it is not the same organ.
Prostate cancer in females is extremely rare in medical history. When it occurs, care often needs specialists. Treatment may include surgery such as a prostatectomy or targeted therapy guided by marker levels.
Keeping track of symptoms and distinguishing common issues like prostatitis from rare malignancy helps protect long-term health. Ongoing research continues to refine detection and therapy for both men and females throughout life.




