Do Women Have a Prostate? Exploring the Female Anatomy
Understanding the Female “Prostate” and Its Role
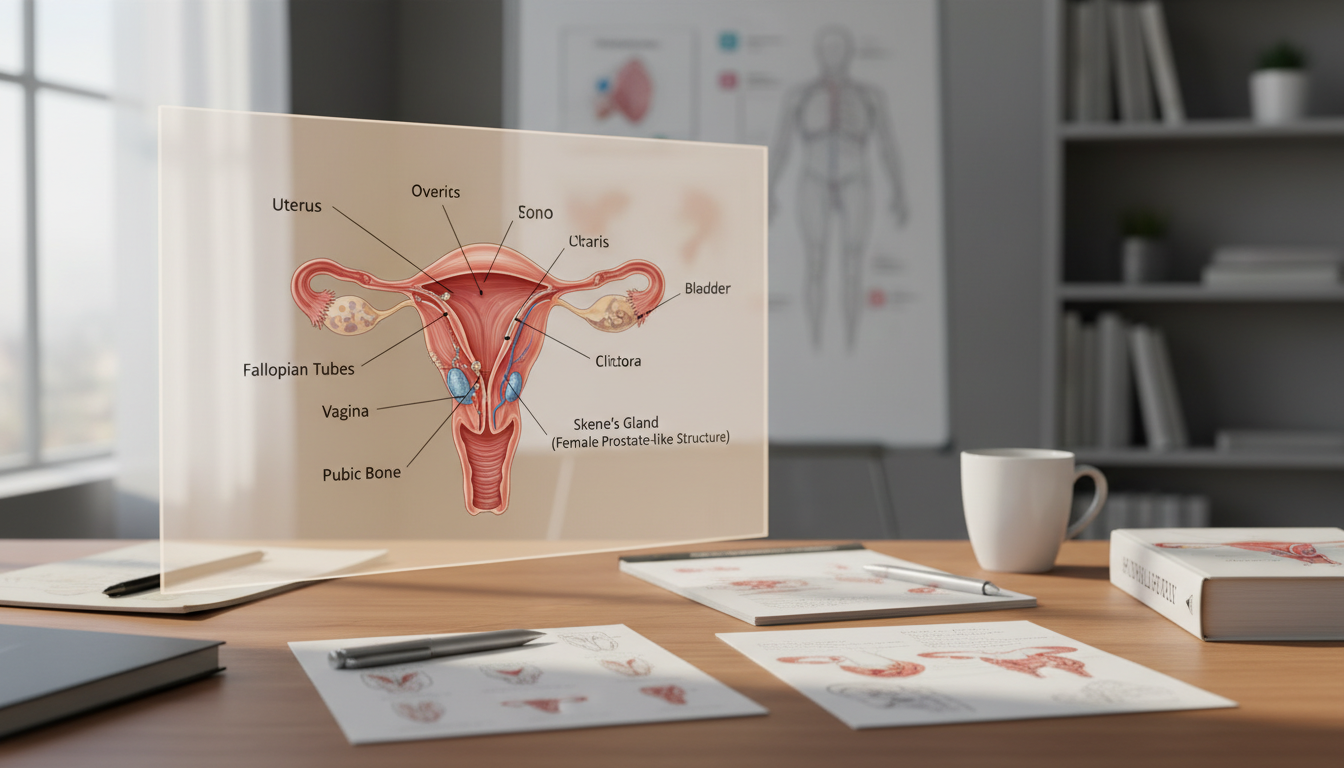
Could a part of the human body stay hidden for years due to its label? Many people feel doubt when they look for medical information on this specific organ.
While some sources say it is not there, leading journals suggest otherwise. This study looks at the prostate version existing in the female frame.
Knowing facts helps finding health issues soon. This look gives the clarity needed for medical growth. Our goal is to provide reliable information for every reader to help them understand their health.
Key Takeaways
- Research into this medical inquiry reveals surprising biological facts.
- Medical sources often provide conflicting data regarding women and their health.
- Skene’s glands serve as the functional version in the female frame.
- Early growth shows that both sexes share similar biological origins.
- Knowing these structures helps in finding urological and health issues.
- Accurate knowledge promotes better screening, care, and total wellness.
Understanding the Male Prostate: A Foundation
The male prostate is a small yet vital organ that plays a central role in the reproductive health of men. This walnut-shaped organ creates the fluids necessary for successful reproduction. Understanding its biology helps clarify why similar structures exist in different bodies.
What Is the Prostate Gland?
The prostate gland is a key reproductive organ in males. It primarily produces prostatic fluid, which makes up a large portion of seminal fluid. This fluid protects and nourishes sperm cells during their journey.
Physicians describe the prostate as a muscular and glandular structure. It serves several essential roles, including:
- Providing alkaline fluid to neutralize vaginal acidity.
- Helping to transport sperm through the reproductive tract.
- Supporting the overall survival of healthy sperm.
Location and Anatomy of the Male Prostate
The male prostate sits in a very specific spot within the pelvis. It is located just below the bladder and sits in front of the rectum. Because of this location, doctors can easily examine the gland during routine medical checkups.
The prostate surrounds the upper part of the urethra. This is the tube that carries urine out of the bladder. Because the tissue wraps around this tube, any changes in the prostate size can affect how a person urinates.
Functions and Clinical Significance
The main function of the prostate is the secretion of enzymes and proteins. One critical protein is the prostate-specific antigen. Most doctors refer to this simply as psa when performing screenings for cancer.
As men age, the prostate can develop different conditions. Common issues include benign growth or prostatitis, which is an inflammation of the gland. High levels of certain biomarkers often signal that the male prostate requires medical attention.
The prostate serves as a biological powerhouse, ensuring the viability of the male reproductive process through precise chemical secretions.
This foundational knowledge of male anatomy allows researchers to better understand the shared embryologic origins of reproductive structures. By viewing the prostate as both a functional and clinical landmark, we can better explore its counterparts in all human bodies.
| Feature | Description | Clinical Significance |
|---|---|---|
| Physical Shape | Walnut-shaped | Standard reference for healthy size |
| Fluid Output | Prostatic Fluid | Essential for sperm nourishment |
| Key Biomarker | PSA protein | Early indicator of cancer presence |
| Main Risks | Inflammation | Leads to common issues like prostatitis |
Do Women Have a Prostate? The Answer Explained
Many people are surprised to learn that the female body contains a functional counterpart to the male prostate gland. While females do not have the exact same large organ found in men, they possess a specialized set of tissues. These structures are known as the skene glands.
Historically, medical textbooks often overlooked these small glands. However, modern research confirms that women do have an anatomical equivalent that performs similar roles. This discovery has changed how scientists view the internal prostate system across different genders.
The Skene’s Glands: Female Prostate Equivalent
The skene glands, often called the paraurethral glands, serve as the widely recognized female prostate. Although they are much smaller than the male version, these structures share many anatomical traits. They are located near the lower end of the urethra, where they play a vital role in the reproductive anatomy.
These glands are not just minor features of the anatomy. They produce specific proteins, such as prostate-specific antigen (PSA), which was once thought to only exist in men. This shared function is why many experts now use the term women prostate when discussing this part of the reproductive system in women.
Embryological Development and Shared Origins
The reason for this striking similarity lies in how a fetus develops before birth. Both the male prostate and the female prostate grow from the same embryonic tissue. This source material is called the urogenital sinus, which acts as a blueprint for several organs.
In the early stages of life, the precursor for these glands is identical. As the fetus grows, hormones guide the development of these structures based on biological sex. In males, the prostate grows larger to support the transport of fluid. In females, the same tissue forms smaller clusters that maintain similar chemical properties.
Understanding this connection helps doctors provide better care for women. It highlights that while the size and shape differ, the biological foundation remains the same. Recognizing these similarities ensures that we treat the human body with a complete and accurate perspective.
| Feature | Male Prostate | Female Prostate (Skene’s) |
|---|---|---|
| Embryonic Origin | Urogenital Sinus | Urogenital Sinus |
| Primary Secretions | PSA and PAP | PSA and PAP |
| Relative Size | Larger (Walnut-sized) | Smaller (Microscopic to pea-sized) |
| Location | Below the bladder | Along the urethra |
Anatomy and Location of the Female Prostate
Identifying the precise location of the Skene’s glands is the first step in recognizing their importance to female reproductive health. These structures sit within the anterior vaginal wall near the lower end of the urethra. This specific area often generates interest due to its link to sexual wellness and internal sensitivity.
Historically, researchers overlooked these glands because of their small size. However, modern medicine now recognizes them as a functional and biological counterpart to the male prostate. Understanding where they reside helps clarify many aspects of female physiology.
Where Are Skene’s Glands Located?
The skene glands open directly into the urethra and sit adjacent to the external opening. This part of the female anatomy mirrors the way the male prostate surrounds the urinary tract in men. Doctors emphasize that these are secretory organs rather than simple components of the urinary system.
Each skene gland exists in the anterior vaginal region, tucked just behind the pelvic bone. Their placement on the vaginal wall allows them to be stimulated during physical activity. This location makes them a key component of the internal reproductive landscape.
“The G-spot is a sensitive area on the anterior vaginal wall linked to the urethra and its surrounding tissues near the bladder neck.”
Structural Composition and Size
While the male prostate is about the size of a walnut, the female equivalent is much smaller. The skene glands consist of complex glandular tissue and small ducts. These ducts allow for the release of specific fluids during moments of arousal.
Even though the size is different, the anterior vaginal structures share the same cellular makeup as the male version. This makes the anterior vaginal wall a focal point for medical study regarding prostate-specific antigens. The tissue of each gland is delicate and reacts to hormonal changes over time.
The vaginal wall provides support for these tiny structures. Each individual gland plays a role in the local environment. Professionals observe that the wall itself can feel different when these tissues are active. Furthermore, the surrounding wall structure contains many blood vessels that support glandular health.
| Feature | Male Prostate | Female Prostate (Skene’s) |
|---|---|---|
| Primary Location | Surrounding the bladder neck | Along the anterior vaginal wall |
| Average Size | Roughly the size of a walnut | Microscopic to pea-sized |
| Main Function | Producing seminal fluid | Secretion of lubricating fluids |
| Urethral Connection | Wraps around the tube | Opens into the tube |
Why Skene’s Glands Are Called the Female Prostate
The term “female prostate” is more than just a nickname; it reflects deep-rooted biological parallels found in the skene glands. For decades, medical texts focused primarily on the male version of this organ. However, researchers now recognize that women possess a nearly identical equivalent that shares its embryological origin and role within the body.
By looking at the biochemical markers and cellular makeup, we can see why these glands female prostate are so unique. This recognition has significant implications for how we treat urological health in women. It changes the way we view human anatomy and clinical diagnostics for better patient care.
Biochemical Similarities: PSA and PAP Production
One of the most compelling reasons for this name is the presence of prostate-specific antigen (PSA). Traditionally, doctors used psa levels strictly to screen for health issues in males. However, recent studies have confirmed that the skene glands female also produce this specific protein in measurable amounts.
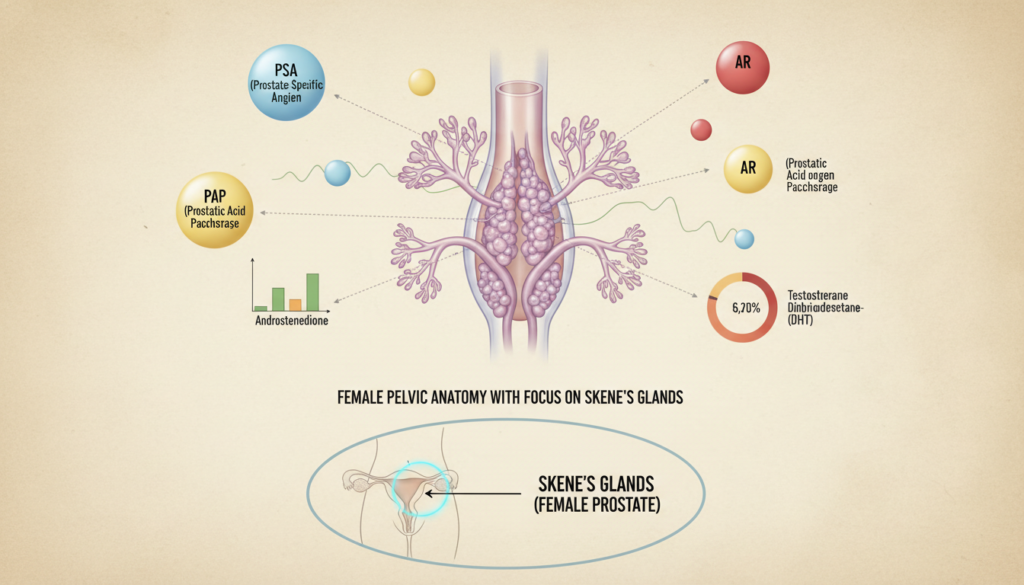
In addition to psa, these glands secrete prostatic acid phosphatase (PAP). This enzyme was once thought to be exclusive to the male prostate. Finding these markers in the female prostate revolutionized our understanding of the skene glands and their complex secretory role. Biochemical evidence provides the strongest link between these two structures.
Tissue Architecture and Glandular Structure
When we examine the tissue under a microscope, the similarities between the sexes become even more apparent. The skene glands female consist of a complex network of tiny ducts and secretory cells. This anatomy mirrors the internal structure found in the male prostate, showing a shared biological blueprint.
These glands female are surrounded by smooth muscle, which helps with their daily secretory function. Although they are much smaller than the version found in males, their histological design is virtually the same. The glands use the same cell types to create and transport fluids through the body.
Functional Parallels Between Male and Female Prostate
There are clear functional similarities between these two organs. Both systems are closely linked to the urinary tract and play a role in overall reproductive health. They both produce secretions that provide antimicrobial protection for the urethra, helping to prevent infections in the female prostate area.
Scientific studies suggest that the function of the glands female prostate may also be involved in the sexual response. While the male prostate is larger and more central to reproduction, the glands female remain essential for local health. Recognizing this helps doctors provide more accurate information to their patients.
The recognition of the female prostate is a vital step toward gender-inclusive medicine and improved urological research.
Comparison of the Male and Female Prostate
| Feature | Male Prostate | Female Prostate (Skene’s) |
|---|---|---|
| Biomarkers | Produces PSA and PAP | Produces PSA and PAP |
| Tissue Type | Glandular and Ductal | Glandular and Ductal |
| Primary Role | Reproductive Secretions | Antimicrobial Protection |
| Urethral Link | Surrounds Urethra | Parallel to Urethra |
Can Women Get Prostate Cancer?
Addressing the possibility of prostate cancer in women requires a look at both males statistics and rare female anatomical conditions. While the gland is primarily associated with men, medical science shows that a female equivalent exists. This knowledge helps clarify how specific malignancies can affect different bodies.
Prostate Cancer in Men: An Overview
Prostate cancer remains one of the most common forms of cancer among males. Statistics show that roughly 1 in 8 men receive a prostate cancer diagnosis during their lifetime. Fortunately, this condition is highly manageable when doctors find it early through routine screening of the prostate.
Some low-risk cases require no immediate treatment at all. Instead, doctors use active surveillance to monitor the prostate without invasive surgery. For others, advanced therapy options provide effective solutions for prostate cancer. Typical risk factors for men include:
- Advanced age (usually over 50)
- A history of prostate cancer in the family
- Genetic mutations like BRCA1 or BRCA2
| Approach | Description |
|---|---|
| Focal Therapy | Includes cryotherapy or HIFU to target specific areas of prostate cancer. |
| Radical Prostatectomy | The surgical removal of the prostate to eliminate prostate cancer. |
Skene’s Gland Carcinoma: The Female Equivalent
Can a person without a male reproductive system actually get prostate cancer? The technical answer is yes, although it is exceptionally rare. This specific cancer develops in the skene gland, which sits near the bladder and urethra. Experts note that these glands produce the same biochemical markers as the male organ.
Medical experts refer to this condition as skene gland carcinoma. Because these glands share embryological origins with the male prostate, they represent the female version of the organ. A diagnosis of this type requires specialized treatment to protect female health.
“There have only been 20 reported cases of Skene’s gland carcinoma throughout scientific literature.”
While prostate cancer is a major concern for many, this rare female condition remains a statistical anomaly. Understanding these functional parallels helps doctors improve overall health outcomes and diagnostic accuracy. Early treatment and screening ensure the best results for any patient facing a prostate cancer diagnosis.
Common Misconceptions About the Female Prostate
Breaking down the walls of misinformation requires a closer look at the Skene’s glands and their vital role in women’s health. Many people hold outdated views because of historical gaps in medical research and cultural taboos. These gaps often leave providers with insufficient education regarding female anatomy.
Understanding this area of the body is essential for effective therapy. When providers ignore these structures, they may overlook the root cause of pelvic dysfunction. Specialized therapy can help manage various conditions that affect the female pelvic region.
Misconception 1: Only Men Have a Prostate
The most widespread myth is that the prostate is a uniquely male organ. While women do not have the exact same large gland as men, they possess a functional equivalent. The skene gland system represents the female version of this tissue.
Medical studies show that women have glands that develop from the same embryonic roots as the male prostate. Calling it the women prostate helps clarify its biological origin. This naming way recognizes that both sexes share similar glandular structures.
Misconception 2: The Female Prostate Serves No Important Function
Some believe the female prostate is just a vestigial remnant with no real function. This is incorrect, as the skene glands help protect the urethra from infections. They also produce secretions that contribute to urogenital health and sexual response.
These glands sit near the pelvic muscles and play a part in overall pelvic stability. If they become inflamed, it can lead to physical dysfunction or pain. Targeted physical therapy often focuses on the muscles surrounding these structures to alleviate discomfort from various conditions.
Misconception 3: Women Cannot Develop Prostate Cancer
Many believe women are immune to prostate-related cancer. Although it is extremely rare, cancer can develop in the skene gland. Medical literature has documented about 20 cases of this specific cancer.
Because the women prostate produces PSA, doctors can sometimes use similar markers for diagnosis. Understanding that this prostate tissue exists allows for better screening. Early detection is key to treating any form of cancer effectively.
The G-Spot and Female Prostate: Understanding the Connection
In 1950, Ernst Gräfenberg described a sensitive area on the anterior vaginal wall. Modern studies suggest this “G-spot” is actually the female prostate and its surrounding muscles. The debate over whether the G-spot is a distinct anatomy is often just a way of describing the same region near the urethra.
Focusing on the women prostate provides a scientific basis for the female orgasm. Statistics show that an orgasm can occur through different pathways. While some reach orgasm through penetration, many require clitoral stimulation to achieve orgasm.
The shift from mythologized concepts to anatomical reality helps providers offer better therapy for sexual dysfunction.
Research indicates that 40.9% of subjects experience orgasm through both clitoral and vaginal stimulation. Another 35.4% reach orgasm through clitoral contact alone. Only 20.1% reported an orgasm from vaginal stimulation by itself, emphasizing that the clitoris remains the primary orgasm source for 70-80% of people.
| Type of Orgasm Stimulation | Percentage of Women | Key Anatomical Focus |
|---|---|---|
| Combined Clitoral & Vaginal | 40.9% | Clitoris and Skene’s Glands |
| Clitoral Only | 35.4% | External Clitoral Glans |
| Vaginal Only | 20.1% | Anterior Vaginal Wall |
Conclusion
The historical debate over whether females possess a prostate-like structure has finally reached a scientific consensus. While women do not have the exact same organ as men, the female prostate exists in the form of the Skene’s glands. These glands sit near the urethra and share a similar anatomy with the male version.
They develop from the same tissue, marking an important part of human development. Modern review articles and studies with a registered doi highlight the biochemical traits of these structures. These glands produce PSA, a protein once thought to only exist in men.
This information changed how people view the female body and its health needs. Throughout history, medical review papers have tracked this evolution in understanding. Documentation found under a specific doi often cites these findings to validate clinical practices.
Recognizing the women prostate is more than just a naming exercise. It helps in the treatment of certain conditions, such as prostatitis or pelvic dysfunction. Issues in this area can affect the bladder or pelvic muscles.
Using targeted therapy often leads to better results for women. Clinicians use a doi to access the latest research on these therapies. Medical experts now link these structures to the female orgasm and general sexual well-being.
A doi search reveals many papers discussing how dysfunction here impacts quality of life. Understanding how an orgasm involves these tissues provides a clearer picture of sexual function. Knowing your own history and biology is the best method to manage your wellness.
Each study in medical history points toward a more inclusive view of prostate wellness. This knowledge empowers females to advocate for themselves during checkups. Understanding these prostate issues ensures that no aspect of the females reproductive system is ignored.
Professional guidance remains the most reliable way to address any prostate or pelvic therapy concerns. Individual health matters, and expert advice provides the clearest path forward for any patient.
